Introduction
A 58-year-old office worker with years of low back pain now experiences leg numbness and difficulty walking. MRI reveals degenerative disc disease at L4-L5 with loss of disc height, foraminal stenosis, and grade I spondylolisthesis. Conservative treatment has failed. The surgeon recommends spinal fusion. At the center of the operation is an interbody cage, a small implant placed between vertebrae after disc removal. The procedure, known as back fusion with cage, restores alignment and creates the environment for bone healing. One specific approach, lumbar cage fusion posterior (PLIF), accesses the spine from the back, allowing both decompression and cage insertion through a single incision. This article explains how these technologies work, when they are indicated, and what outcomes patients can expect.
What Is an Interbody Cage and Why Is It Essential?
The Problem Without a Cage
When a degenerated or herniated disc is removed, the intervertebral space collapses. Collapse leads to foraminal narrowing, nerve root compression, and loss of spinal alignment. Simply placing bone graft without structural support results in graft resorption and pseudoarthrosis. The interbody cage solves these problems by acting as a structural spacer that maintains disc height and lordosis while protecting the bone graft.
Materials and Design Evolution
Early cages were cylindrical titanium mesh devices. Modern interbody cages come in multiple materials: PEEK (polyetheretherketone) has a modulus similar to bone, reducing subsidence; titanium cages with 3D-printed porous surfaces promote osseointegration; allograft or biodegradable cages offer graft-only options. Anatomical footprints match the vertebral endplate shape, maximizing surface area. Many cages feature radiopaque markers for X-ray visualization, large central windows for graft packing, and lordotic angles (4-12°) to restore sagittal balance.
Graft Materials Packed Inside the Cage
The cage itself does not fuse bone—it contains and protects the graft. Options include autograft (from the patient’s iliac crest or local lamina), allograft (donor bone), demineralized bone matrix (DBM), calcium phosphate ceramics, or bone morphogenetic protein (BMP). Autograft remains the gold standard but adds donor site morbidity. BMP provides osteoinduction but carries a risk of heterotopic ossification and is expensive.

How Does Back Fusion with Cage Work in Practice?
Indications for Back Fusion with Cage
A back fusion with cage procedure is indicated for several spinal disorders: degenerative disc disease with intractable axial pain, spondylolisthesis (isthmic or degenerative), recurrent disc herniation after failed microdiscectomy, spinal stenosis with instability, pseudoarthrosis from prior fusion, and certain fractures or tumors. Patients typically have failed at least six months of nonoperative care, including physical therapy, medications, and epidural injections.
The Surgical Steps
The operation is performed under general anesthesia. Through a midline posterior incision, the surgeon exposes the lamina and facet joints. A laminectomy decompresses the spinal canal. Facetectomy (partial or complete) allows access to the disc space. The disc is removed using rongeurs and endplate scrapers. Cartilage is cleared down to bleeding bone—critical for fusion. The appropriately sized interbody cage, packed with bone graft, is inserted into the disc space. Supplemental pedicle screw fixation (usually bilateral at the fused levels) provides immediate stability. The wound is closed over drains.
Clinical Outcomes and Fusion Rates
Large series report fusion rates of 85-95% for single-level back fusion with cage procedures. Clinical success (significant improvement in pain and function) ranges from 70-85%. The average hospital stay is 2-4 days. Return to light work occurs at 6-12 weeks; heavy labor may require 4-6 months. Patient satisfaction rates exceed 80% at two-year follow-up.

What Is Lumbar Cage Fusion Posterior (PLIF) and How Does It Differ?
PLIF Defined
Lumbar cage fusion posterior, also known as Posterior Lumbar Interbody Fusion (PLIF), is a specific technique for inserting the cage from a posterior approach. It differs from TLIF (Transforaminal Lumbar Interbody Fusion), which accesses the disc space through a more lateral trajectory, and ALIF (Anterior Lumbar Interbody Fusion), which approaches from the front. PLIF requires bilateral facetectomy to expose the disc, allowing two cages (left and right) to be placed.
Advantages of the PLIF Approach
PLIF provides direct, wide visualization of the spinal canal and nerve roots, making it ideal for patients with central stenosis or bilateral symptoms. The same incision allows thorough decompression and cage insertion without repositioning the patient. Pedicle screws are easily added through the same approach. PLIF restores disc height and lordosis effectively, and the bilateral cage placement provides symmetric support.
Disadvantages and Complications
PLIF requires more retraction on the nerve roots than TLIF, increasing the risk of postoperative radiculitis (5-10%) and dural tear (2-5%). Removing both facet joints can destabilize the segment, making pedicle screw fixation mandatory. Cage subsidence occurs in 5-10% of cases, especially in osteoporotic bone. Infection rates are 1-3%. Despite these risks, PLIF remains a workhorse technique for lumbar fusion.
Clinical Scenario – The Patient with L4-L5 Spondylolisthesis
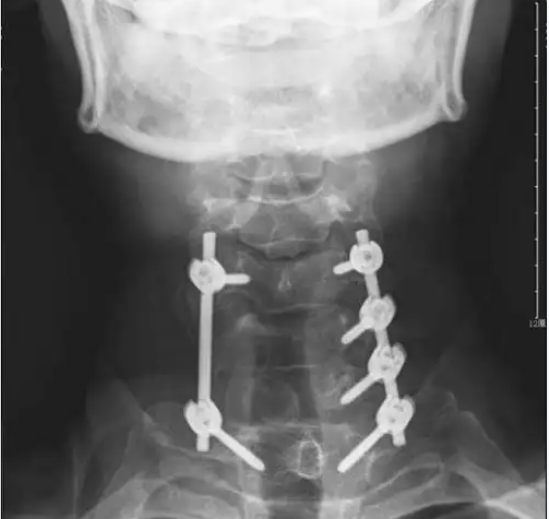
A 62-year-old with degenerative spondylolisthesis at L4-L5 and symptomatic stenosis undergoes a lumbar cage fusion posterior (PLIF). Bilateral laminectomy and facetectomy decompress the thecal sac and nerve roots. Two PEEK cages packed with local autograft are inserted into the disc space from left and right. Pedicle screws and rods are placed at L4-L5. Postoperative X-rays show restored disc height and normal alignment. The patient wears a brace for 6 weeks and returns to walking at 2 weeks. At one year, the fusion is solid, and leg pain is resolved.
Comparing Surgical Approaches: PLIF vs. TLIF vs. ALIF
Key Differences at a Glance
PLIF (posterior): Bilateral facetectomy, two cages, direct nerve root retraction. Best for central stenosis.
TLIF (transforaminal): Unilateral facetectomy, single larger cage, less nerve retraction. Preferred for unilateral symptoms or revision cases.
ALIF (anterior): No posterior muscle dissection, large cages, better lordosis restoration. Requires access surgeon, risks vascular injury.
Evidence for PLIF in 2025-2026
Recent meta-analyses show no significant difference in fusion rates between PLIF and TLIF (approximately 90% for both). TLIF has a lower risk of postoperative radiculitis (3% vs. 7%) and shorter operative time. PLIF offers better direct decompression for central stenosis. The choice often depends on surgeon preference and specific pathology. Minimally invasive PLIF techniques using tubular retractors are gaining adoption, reducing blood loss and hospital stay.
Conclusion
The interbody cage is a cornerstone of modern spinal fusion. Back fusion with cage procedures reliably treat degenerative disc disease, spondylolisthesis, and instability. Lumbar cage fusion posterior (PLIF) provides a time-tested, effective approach that combines decompression and fusion through a single posterior incision. With proper patient selection, meticulous technique, and appropriate graft material, these procedures achieve high fusion rates and excellent clinical outcomes. Advances in cage materials (PEEK, titanium, 3D-printed porous designs) and minimally invasive techniques continue to improve patient recovery. For patients with chronic disabling back or leg pain from spinal disorders, interbody cage fusion remains a proven, reliable solution.




