Introduction
A 7-year-old child with congenital femoral deficiency faces a lifetime of limb length discrepancy. A 34-year-old truck driver sustains an open tibial fracture with bone loss and infection. A 22-year-old with Blount’s disease develops progressive varus deformity. These seemingly unrelated conditions share a common solution: distraction osteogenesis using a ring fixator. The ilizarov external fixator, pioneered by Gavriil Ilizarov in the 1950s, introduced the biological principle that gradual distraction of a bone cut creates new bone formation. Modern fixator ilizarov systems have expanded to treat nonunions, bone defects, limb length discrepancy, and complex deformities. This article reviews the science, surgical techniques, and clinical outcomes of circular external fixation.
The Biology of Distraction Osteogenesis
What Happens When You Distract a Bone Cut?
The ilizarov external fixator is based on a simple but profound discovery: when a bone is cut (corticotomy) and gradually pulled apart at a rate of 1 mm per day, new bone forms in the gap. This process, called distraction osteogenesis, involves three phases: latency (5-7 days for callus formation), distraction (1 mm/day in 4 increments), and consolidation (months for new bone to mineralize). The ring fixator provides the stable, adjustable frame necessary for precise control.
Why Tensioned Wires Matter
A key innovation of the fixator ilizarov is the use of thin (1.5-1.8 mm) transosseous wires tensioned to 90-130 kg. Tensioned wires convert the ring fixator into a stiff, stable construct despite the small wire diameter. The wires cross at angles, creating a “tent” that resists axial, bending, and torsional loads while allowing micromotion that stimulates healing. This biomechanical property distinguishes the ilizarov external fixator from other external fixators.
Soft Tissue Response
Gradual distraction also affects soft tissues. Nerves, vessels, and muscles lengthen at rates comparable to bone when done slowly. This biological advantage makes the ring fixator ideal for limb lengthening—up to 8-10 cm can be achieved in the femur or tibia without permanent nerve damage.

Clinical Applications of the Ring Fixator
Limb Lengthening
The ring fixator is the gold standard for limb length discrepancy (LLD). Congenital conditions (proximal femoral focal deficiency, fibular hemimelia), post-traumatic growth arrest, and post-infectious bone loss are common indications. The ilizarov external fixator allows lengthening of 1-2 mm per day in the tibia and 1 mm per day in the femur. Total lengthening up to 8 cm is safe. Complications include pin tract infection (common but rarely serious), joint contracture (preventable with physical therapy), and regenerate fracture (rare).
Deformity Correction
Angular deformities (varus, valgus, procurvatum, recurvatum) can be corrected using a fixator ilizarov with hinged rings. The frame is constructed with a hinge at the apex of the deformity. Gradual opening of the hinge corrects the angle while maintaining bone contact. Multiapical or rotational deformities require more complex frame constructs. Computer-assisted hexapod systems (e.g., Taylor Spatial Frame) have simplified complex corrections but remain based on the ring fixator principle.
Nonunion and Bone Defect Treatment
Hypertrophic nonunions respond to compression with the ilizarov external fixator. Atrophic nonunions and infected nonunions require debridement, bone transport, or the “docking” technique. Bone transport involves moving a segment of bone (transport disk) across a defect using the ring fixator. New bone forms behind the moving segment (regenerate), and the transported segment docks at the opposite side. Success rates for bone transport exceed 90% for defects up to 6-8 cm.
Clinical Scenario – Post-Traumatic Tibial Bone Defect
A 40-year-old sustains a Gustilo IIIB open tibial fracture with 5 cm of bone loss. After debridement and soft tissue coverage, a ring fixator is applied. A proximal corticotomy is performed. Distraction begins at 1 mm/day. The transport disk moves distally, and new bone forms in the proximal gap. After 50 days, the transport disk docks with the distal fragment. Compression is applied at the docking site. The total frame time is 8 months. Radiographs show healed regenerate and docking site. The patient returns to walking without limb length discrepancy.
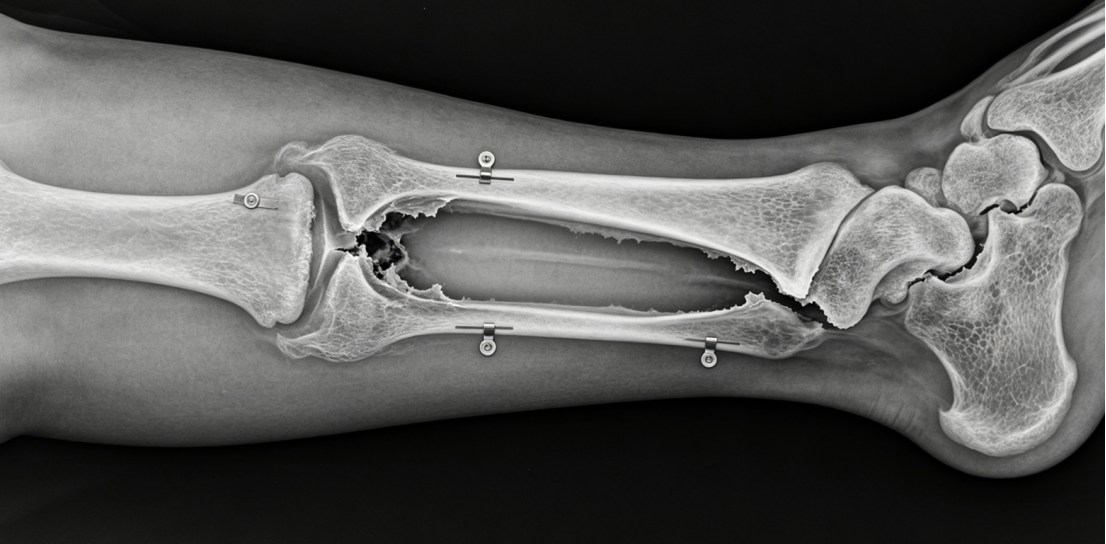
Fixator Ilizarov in Complex Foot and Ankle Pathology
Charcot Foot Reconstruction
Diabetic patients with Charcot neuroarthropathy develop midfoot collapse, rocker-bottom deformity, and ulceration. The ilizarov external fixator allows gradual correction of the deformity while maintaining soft tissue integrity. A ring fixator applied to the foot and ankle can compress the Charcot joint, realign the arch, and protect the plantar surface. Ulcers heal after offloading. Fusion rates of 70-80% are reported, with limb salvage rates exceeding 90%.
Ankle Arthrodesis in Infected or Osteoporotic Bone
Traditional ankle fusion with plates and screws fails in infected or severely osteoporotic bone. The fixator ilizarov provides compression across the tibiotalar joint without hardware in the infected field. A ring fixator spanning the ankle is applied. Compression of 1-2 mm is performed daily for several days. Union rates exceed 85% even in complex cases. The frame is removed after 12-16 weeks.
Equinus Deformity Correction
Equinus (toe-down deformity) from cerebral palsy, stroke, or trauma can be corrected gradually with a ring fixator. A hinged frame across the ankle is distracted anteriorly, lengthening the Achilles tendon and posterior capsule without open surgery. Pin site care and physical therapy are essential.
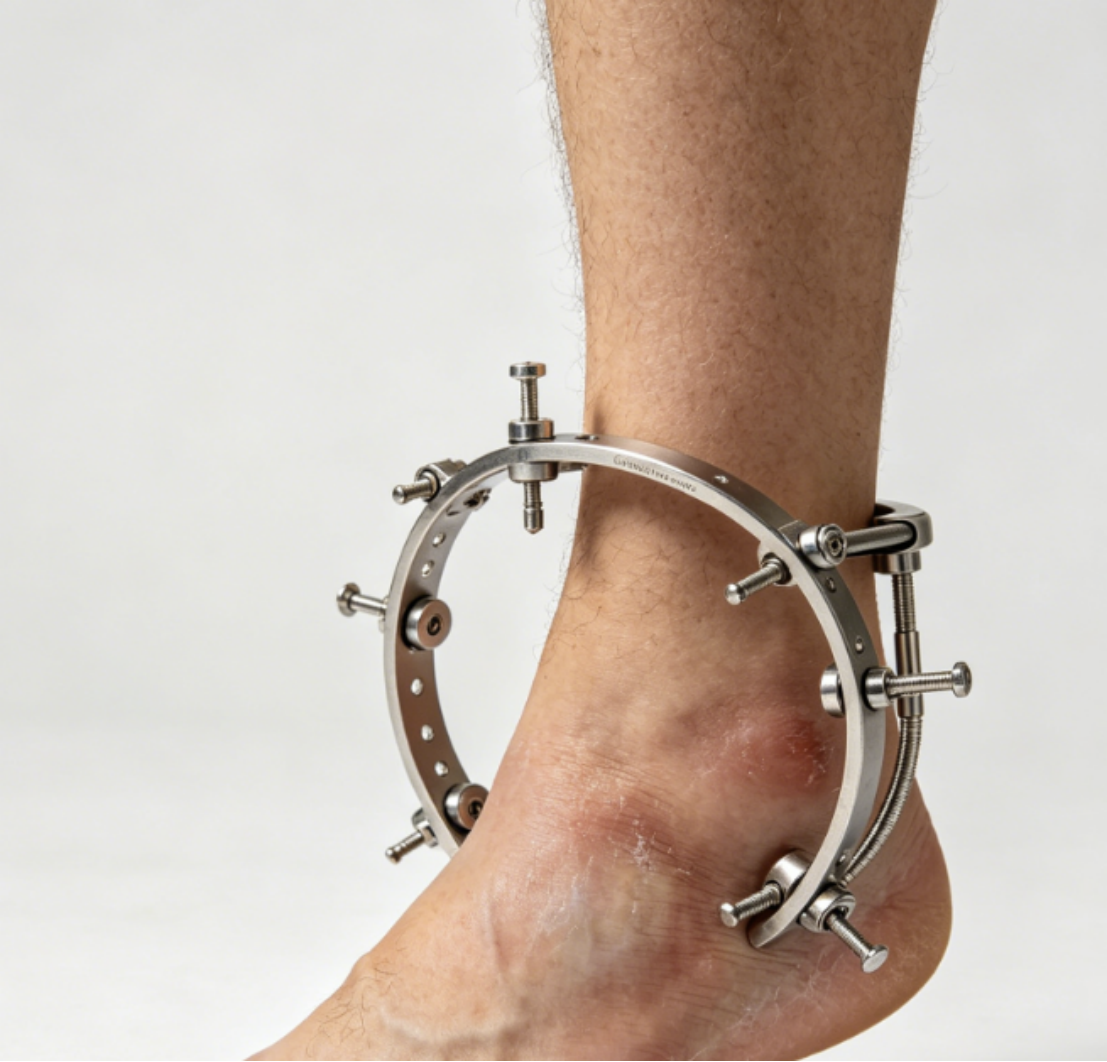
Complications and Management
Pin Tract Infection
Pin tract infection is the most common complication, affecting 20-60% of patients. Most are superficial and respond to oral antibiotics and pin site care (daily cleaning with chlorhexidine). Deep infection requiring pin removal occurs in <5% of cases. Using olive wires (which increase contact area) reduces infection risk.
Joint Contracture
Knee or ankle contractures develop in 10-30% of patients undergoing limb lengthening. Prevention includes aggressive physical therapy, splinting, and maintaining full range of motion during distraction. If contracture occurs, the ring fixator can be hinged to simultaneously lengthen and correct joint position.
Regenerate Fracture
Fracture through the new bone (regenerate) occurs in 2-5% of cases, usually after frame removal when the bone is still weak. Premature frame removal (before regenerate consolidation on X-ray) is a risk factor. Treatment involves reframing or casting for 6-8 weeks.
Conclusion
The ring fixator and ilizarov external fixator systems remain indispensable tools for complex limb reconstruction. From congenital deficiencies to post-traumatic bone defects, from diabetic foot collapse to infected nonunions, the fixator ilizarov offers solutions where conventional implants fail. The biological principle of distraction osteogenesis—gradual tension-stress leading to new bone formation—has stood the test of six decades. Modern refinements include hexapod computers, hybrid frames, and patient-specific ring configurations. Surgeons who master the ring fixator can treat conditions that would otherwise lead to amputation or permanent disability.




