Introduction
A 28-year-old driver crashes into a steering wheel, sustaining a tripod fracture of the zygoma, a blowout fracture of the orbital floor, and a depressed frontal bone fracture. Three adjacent but distinct injuries. The reconstructive surgeon must restore the zygomatic prominence, support the globe, and recontour the crnial vault. The zygomatic plate stabilizes the malar eminence. The orbital plate reconstructs the thin floor that protects the eye. The cranial plating system fixes the bone flap and restores forehead contour. This article presents an integrated approach to craniomaxillofacial trauma using these three implant types.
Zygomatic Plate – Restoring the Malar Prominence
Anatomy of Zygomatic Fractures
The zygoma forms the cheek prominence and contributes to the lateral orbital wall and orbital floor. Fractures occur at four points: frontozygomatic suture, infraorbital rim, zygomaticomaxillary buttress, and zygomatic arch. Displacement causes flattening of the cheek, enophthalmos, and trismus. The zygomatic plate is a low-profile, precontoured plate applied to the frontozygomatic region or infraorbital rim.
Surgical Technique
A zygomatic plate is typically placed via an upper blepharoplasty incision (for the frontozygomatic suture) or a subciliary incision (for the infraorbital rim). The plate is contoured to match the patient’s anatomy. Locking screws provide angular stability. Reduction is confirmed by palpation of the malar prominence and intraoperative CT. Union rates exceed 95%, and plate removal is rarely needed.
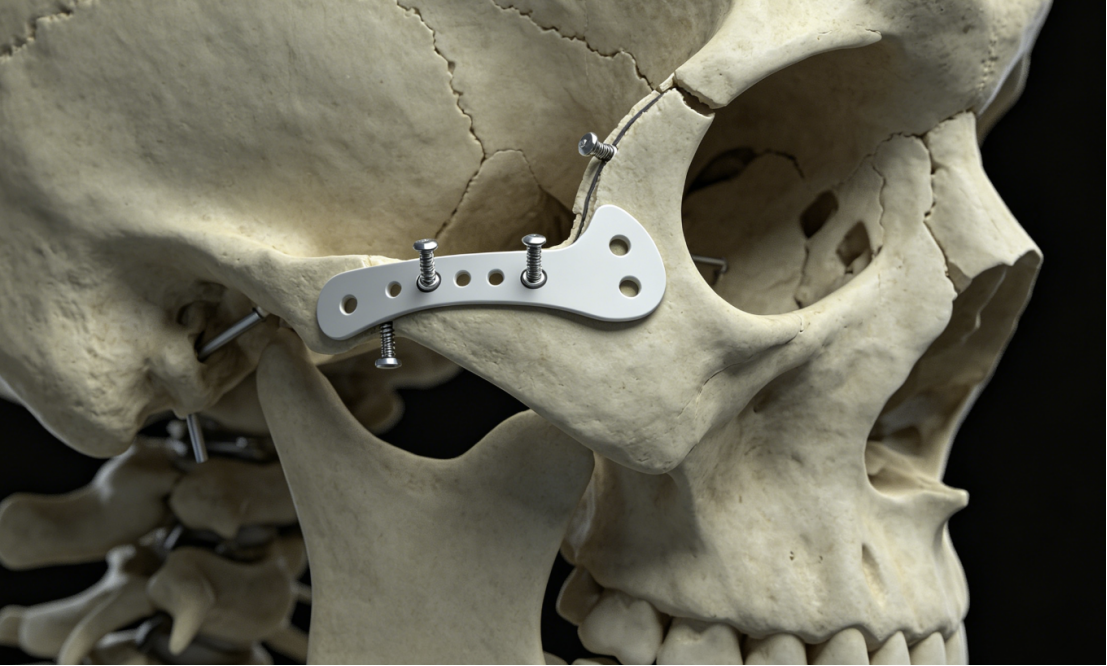
Orbital Plate – Protecting the Globe
Indications for Orbital Plate
Orbital floor fractures with entrapment, enophthalmos >2 mm, or large defects (>2 cm²) require an orbital plate. The implant bridges the defect, prevents herniation of orbital contents, and restores orbital volume. Materials include titanium mesh (strong, easy to contour) and absorbable plates (no secondary surgery, less imaging artifact).
Technical Pearls
The orbital plate is inserted through a transconjunctival or subciliary approach. The plate is placed on the posterior ledge of the orbital floor, not anteriorly where it can impinge on the infraorbital nerve. Screws are optional; many orbital plates are screwless, relying on soft tissue pressure for stability. Postoperative CT confirms plate position. Complications include diplopia (resolves in weeks), implant migration (rare), and infection (<2%).
Image 2 Suggestion: A coronal CT image showing an orbital plate spanning an orbital floor defect. (用作插图)
Cranial Plating System – Restoring the Calvarium
Cranial Plating for Trauma and Craniotomy
The cranial plating system fixes bone flaps after frontal bone fracture repair or craniotomy. Low-profile plates with burr-hole covers restore contour without palpable hardware. Plates are made of titanium or absorbable materials. Dynamic cranial plates that allow for postoperative brain swelling are available for trauma cases.
When to Use Cranial Plates
Indications include depressed skull fractures, frontal sinus fractures with posterior table involvement, and decompressive craniectomy bone flap replacement. The cranial plating system uses 1.5-2.0 mm screws and plates that are malleable but rigid once fixed. Complications are rare but include hardware palpability, infection, and cosmetic deformity from plate prominence.
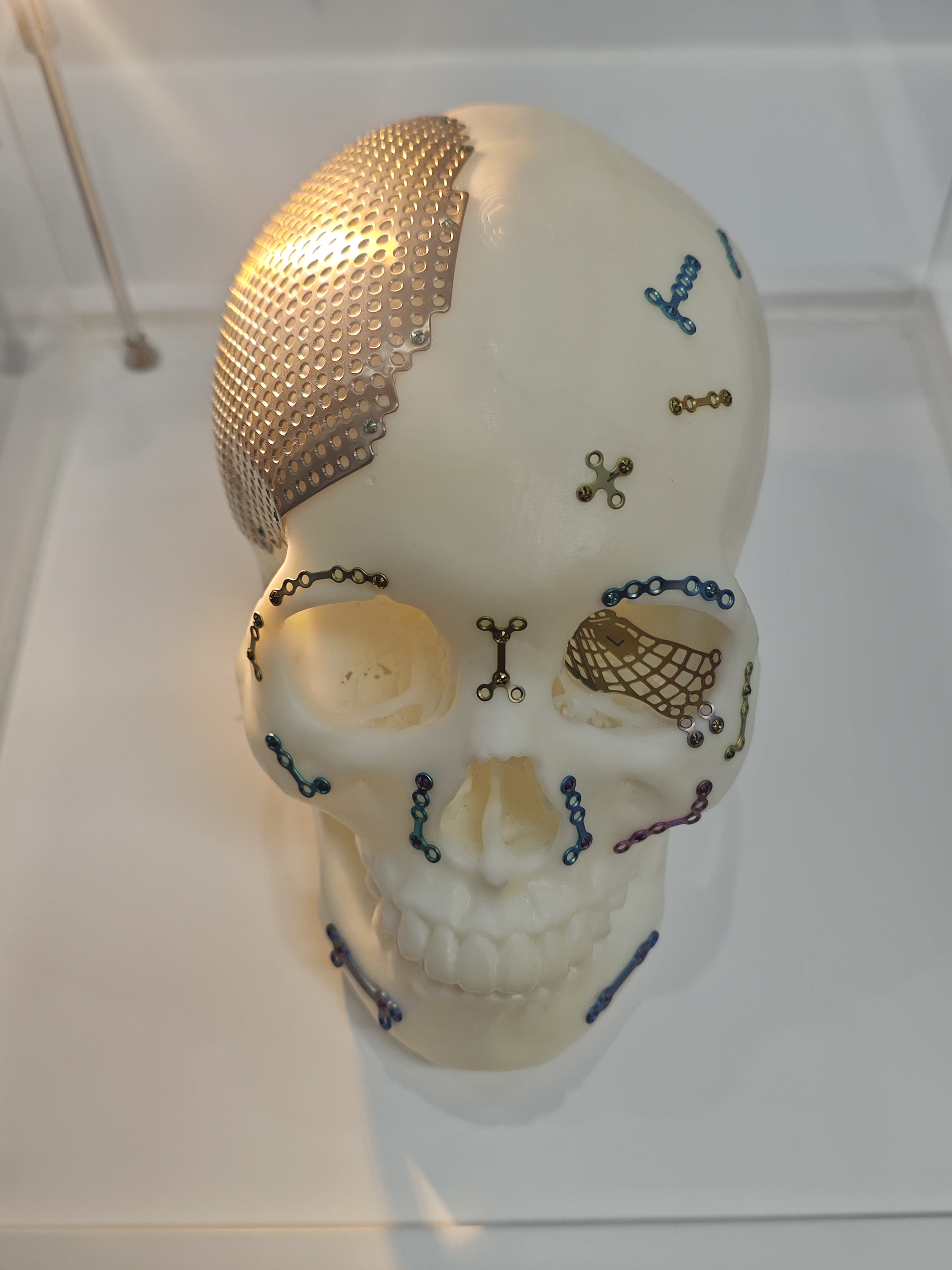
Integrated Approach to Panfacial Fractures
Sequencing the Reconstruction
In panfacial fractures, the order of fixation is critical: (1) cranial plating system to stabilize the frontal bar and establish the vertical dimension; (2) zygomatic plates to restore facial width and projection; (3) orbital plates to correct orbital volume and prevent enophthalmos. This “inside-out, bottom-up” sequence ensures accurate restoration of pre-injury anatomy.
Outcome Expectations
With proper technique, patients return to normal facial contour, eye position, and vision. Hardware-related complications occur in <5% of cases. Most patients do not require implant removal unless symptomatic.
Conclusion
Zygomatic plate, orbital plate, and cranial plating system are essential components of modern craniomaxillofacial trauma surgery. When applied in a coordinated sequence, they restore form and function to the injured face. Advances in precontoured implants, locking screw technology, and intraoperative navigation continue to improve outcomes.




