Introduction
A 28-year-old snowboarder falls onto an outstretched hand, sustaining an intra-articular distal radius fracture. A 55-year-old with a humeral shaft fracture from a bicycle accident needs stable fixation that allows early shoulder motion. A 7-year-old with a femoral fracture after a playground fall requires a growth-friendly, minimally invasive solution. Three different patients, three different fixation needs. The surgeon’s toolkit includes volar plating for the wrist, a humeral nail for the upper arm shaft, and elastic nailing for the child’s femur. Each technique has distinct indications, biomechanical principles, and surgical pearls. This article provides a practical guide to selecting and applying these methods.
When Is Volar Plating the Undisputed Choice for the Distal Radius?
Anatomic and Biomechanical Rationale
The distal radius is the most common fracture site in the upper extremity. Unstable, intra-articular, or dorsally displaced fractures require operative fixation. Volar plating has displaced dorsal plating as the standard because it avoids extensor tendon irritation and provides superior subchondral support. The volar plate is precontoured to fit the palmar concavity, and locking screws placed in the distal row create a fixed-angle construct that supports the articular surface even in osteoporotic bone.
Surgical Approach and Pitfalls
The modified Henry approach between the flexor carpi radialis and the radial artery exposes the distal radius. The plate must be positioned proximal to the watershed line—the ridge where the volar rim meets the articular surface. Placing the plate too distally risks flexor pollicis longus rupture. Intraoperative fluoroscopy confirms screw length; screws penetrating the dorsal cortex can injure extensor tendons. Studies show that volar plating achieves 90-95% good-to-excellent functional outcomes at one year.
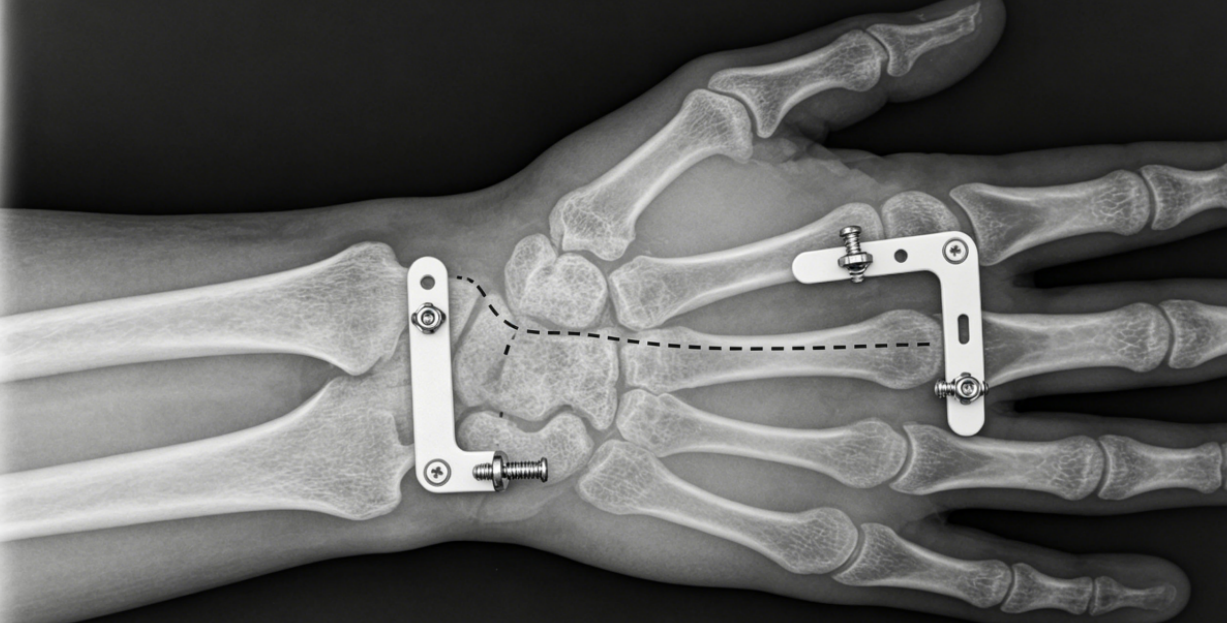
Clinical Scenario – The Active Patient with a Comminuted Fracture
A 45-year-old manual laborer falls from a ladder, sustaining a AO/OTA type C2 distal radius fracture. Volar plating is performed through a flexor carpi radialis approach. The plate is placed proximal to the watershed line, and four distal locking screws capture the articular fragments. Early wrist motion begins at postoperative day three. At six months, the patient returns to heavy lifting with full range of motion and no hardware-related pain.
Why Choose a Humeral Nail for Humeral Shaft Fractures?
Indications and Advantages
Humeral shaft fractures (AO/OTA 12) can be treated with plates or intramedullary nails. The humeral nail offers several advantages: smaller incision, less soft tissue dissection, preservation of the fracture hematoma, and earlier shoulder mobilization. It is particularly useful in polytrauma patients, obese patients, and those with segmental or pathological fractures. The nail is inserted through the proximal humerus, typically via a rotator cuff-splitting approach.
Technical Considerations
Proper entry point is just medial to the greater tuberosity. The nail should be countersunk 5–10 mm below the articular surface to prevent shoulder impingement. Proximal locking screws target the humeral head; distal locking screws are placed using a freehand or electromagnetic technique. Studies report union rates of 90-95% for humeral nailing. Complications include shoulder pain (10-20%), rotator cuff injury, and iatrogenic fracture during insertion.
Clinical Scenario – The Polytrauma Patient with a Humeral Shaft Fracture
A 35-year-old motorcyclist sustains a femoral fracture, a pelvic ring injury, and a closed humeral shaft fracture. Damage control orthopedics prioritizes femoral nailing. For the humerus, a humeral nail is inserted through a small deltoid-splitting approach. The procedure takes 45 minutes with minimal blood loss. The patient begins shoulder pendulum exercises on day one. At three months, the humeral fracture is healed, and the patient has near-normal shoulder function.
*Image 2 Suggestion: An anteroposterior shoulder X-ray showing a humeral nail with proximal and distal locking screws. (用作插图)*
How Does Elastic Nailing Revolutionize Pediatric Fracture Care?
The Concept of Flexible Intramedullary Fixation
Elastic nailing, also known as flexible intramedullary nailing (FIN) or TEN (titanium elastic nail), uses pre-bent titanium nails inserted through the metaphysis. The nails span the fracture site, providing three-point fixation that resists bending and rotation while allowing axial micromotion. This controlled motion stimulates callus formation and accelerates healing. Unlike rigid adult nails, elastic nails do not cross the growth plate, making them safe for skeletally immature patients.
Indications and Contraindications
Elastic nailing is ideal for femoral, tibial, and forearm fractures in children aged 5–15 years. It is indicated for transverse, short oblique, or mildly comminuted fractures. Contraindications include intra-articular extension, wide comminution, and fractures within 2 cm of the physis. The technique is minimally invasive: two small incisions, no periosteal stripping, and rapid recovery. Hospital stay averages 2–3 days, compared to 5–7 days for traction or casting.
Clinical Scenario – The Child with a Femoral Shaft Fracture
An 8-year-old boy falls from a tree, sustaining an isolated midshaft femoral fracture. Elastic nailing is performed under fluoroscopy. Two 3.0 mm titanium nails are pre-bent and inserted from the medial and lateral distal metaphysis. The nails cross the fracture site and engage the proximal metaphysis. Postoperatively, the child is allowed toe-touch weight-bearing with crutches. At six weeks, callus is visible on X-ray, and the child returns to school. Hardware removal is electively performed at six months under brief anesthesia.
Decision Framework – Matching Technique to Patient
Fracture Location and Pattern
Distal radius, intra-articular or unstable → volar plating
Humeral shaft (diaphysis) → humeral nail (or plate, depending on surgeon preference)
Pediatric femoral/tibial/forearm diaphysis → elastic nailing
Patient Age and Bone Quality
Volar plating works well across all ages, with locking screws essential in osteoporotic bone. Humeral nails are suitable for adults of any age, though shoulder impingement risk is higher in very short humeri. Elastic nailing is specifically for children with open physes; it is not designed for adult bone.
Soft Tissue and Comorbidities
Volar plating requires adequate palmar soft tissue coverage. Humeral nails are ideal for obese patients where plate fixation would require extensive dissection. Elastic nailing leaves tiny scars and is well tolerated even in malnourished or multiply injured children.
Conclusion
Volar plating, humeral nailing, and elastic nailing each fill a specific niche in fracture care. Volar plating offers reliable, tendon-sparing fixation for the challenging distal radius. Humeral nails provide a minimally invasive, rapid option for humeral shaft fractures, especially in polytrauma or obese patients. Elastic nailing has transformed pediatric long bone fracture management, allowing early mobilization and excellent healing without physeal damage. By understanding the indications, technical nuances, and limitations of each method, surgeons can deliver optimal, patient-specific care.




